Transitioning From Traditional Arthroscopy Using Nanotechnology in Awake Patient Meniscectomies
By: Vonda J. Wright, M.D., M.S. and Jonathan D. Schwartzman
The pivot from open sports procedures 40 years ago to minimally invasive arthroscopic techniques represents a profound paradigm shift for sports medicine, allowing smaller incision sizes, decreased soft tissue trauma/postoperative pain, faster healing times, lower infection rates and optimized recovery. Minimally invasive sports surgery has been the standard. Now, newer and even smaller diameter visualization scopes are available to achieve these goals while reducing the risk of iatrogenic joint damage during procedures and set the stage for in-office procedures.
Nanotechnology, or needle scopes, allow an incisionless approach with decreased fluid requirements and can be set up in awake patients under local anesthesia. This approach results in rapid recovery for diagnosing and treating meniscus derangements. The 2 mm diameter needle scopes have demonstrated diagnostic and therapeutic efficacy in cases ranging from diagnostic arthroscopy, staging for cartilage procedures, meniscal surgery and elbow/ankle arthroscopy. Like any new approach, transitioning to a new technique creates a learning curve for both the surgeon and operating room staff. The following article outlines transitioning surgical technique from standard arthroscopy to using nanotechnology for awake patient meniscal procedures in an outpatient setting.
Our evolution from standard arthroscopy to NanoScopeTM (Arthrex, Inc.) arthroscopy occurred over four consecutive weeks utilizing a stepwise approach with significant weekly transitions, allowing technical comfort for surgeons and their operating room staff.
Technical Transitions by Week
Week One: The initial transition included the addition of the NanoScope to the normal setup. The NanoScope with 60 cc syringe saline flow is set up and used primarily for the procedure with the traditional scope equipment available as needed. Anesthesia is per the surgeons’ preference, usually general.
The goal of Week One is to use only the NanoScope for the whole procedure without reverting to the standard technique while having it available as rescue.
Week Two: The second transition utilizes only the High Flow 30-degree NanoScope with a 1,000 mililiter saline/pressure bag attached; meanwhile, the 60 cc syringe’s weight moves the NanoScope out of focus. The standard scope equipment is not opened. General anesthesia, or the surgeon’s preference, is utilized once again.
Week Three: After experience with using the NanoScope High Flow 30-degree scope only, local anesthesia with sedation is used as follows:
10 cc, .25 Marcaine, subcutaneous and intracapsule area
20 cc, .25 Marcaine, intra-articular area
Week Four: During the fourth and final week, indicated patients who are deemed safe or able to undergo the procedure under local anesthesia only are scheduled to do so. The operating room is set up as per Week Three. Local anesthesia is switched to 10 cc, 1% Lidocaine and applied to the subcutaneous/intracapsule area to allow for more rapid anesthesia initially, followed by intra-articular 20 cc, .25 Marcaine.
Patients are allowed to bring a playlist of relaxing music of their choice to listen to during the procedure.
Arthroscopy with a NanoScope or needle technology is similar, but not identical to the standard arthroscopic approach. The patient is prepped and draped in the surgeon’s usual manner; in the awake patient, local anesthesia is achieved using a 10 cc injection of 1% lidocaine with epinephrine into the skin and capsule. Once numb, a 20 cc injection of .25% Marcaine is directly injected into the joint. Anatomic landmarks and locations for the point of entry are marked, with the lateral and medial points of entry identified identically to the surgeons’ standard portals. The lateral point of entry is established using a sharp High Flow nanotrocar introduced directly into the notch. The sharp introducer is exchanged for a blunt, plastic-tipped inner stylette and the trocar is advanced carefully into the suprapatellar pouch. The zero-degree trochar is exchanged for the 30-degree nanotrochar over a wire and the NanoScope is introduced.
This step can be eliminated with direct introduction of the curved 30-degree scope if desired. IV tubing attached to a 1,000 cc bag of normal saline with pressure sleeve and fluid added intra-articularly can be used as needed. The NanoScope is then passed into the suprapatellar pouch for examination or per the surgeons’ usual procedure for diagnostic exam. After examining the suprapatellar pouch and medial gutter, the NanoScope is swept into the medial compartment and the medial point of entry is established under direct visualization, first with a spinal needle through which a wire is introduced and over which the point of entry is dilated and the nanoprobe introduced. Meniscal tears are evaluated with the nanoprobe and debrided with straight and curved nanobiters. A 3 mm nanoshaver is then used to complete the meniscectomy as needed. The notch is then examined and probed as is the lateral compartment. As with traditional arthroscopy, the nanoscope is easily switched between lateral and medial points of entry to provide better viewing and access as needed.
Once all compartments are evaluated and meniscal or cartilage work is completed, any fluid and debris is evacuated from the knee and the points of entry are closed with a Steri-Strip and covered with a dressing of choice. Patients are allowed weight bearing as tolerated immediately postoperation with cold therapy as needed. Patients are seen two days postoperation and allowed to return to prior activities at 50% of their presurgical load and advance as tolerated.
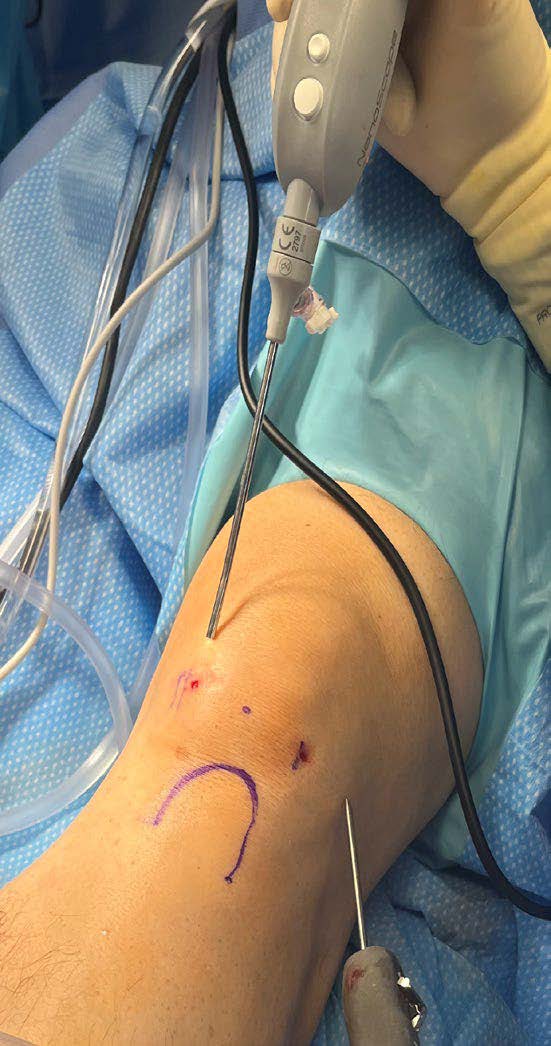
Knee status post-meniscectomy, with the NanoScope instrumentation and 2 mm shaver demonstrating medial and lateral points of entry.
The NanoScope system offers the benefits of minimally invasive arthroscopic procedures while giving surgeons the flexibility to conduct operations in an in-office setting in awake or Monitored Anesthesia Care (MAC)-sedated patients. This flexibility decreases operative time and benefits patients who may experience greater comfort while awake in an in-office setting. Our patients have enthusiastically embraced this approach as they prefer an “incision-less” surgery through points of entry via 1.9 mm needles, no general anesthesia, immediate weight bearing and rapid recovery without the need for postoperative physical therapy or use of postoperative pain medication. For surgeons contemplating a pivot to less invasive techniques, the transition has been easy in our hands and extremely well tolerated by patients.


